Table of Contents
Table of Contents
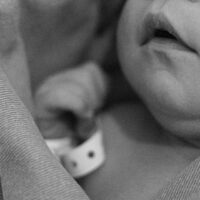 When a newborn shows weakness or limited movement in one arm after delivery, it can be frightening and confusing for parents. One possible cause is a brachial plexus injury, a condition that affects the group of nerves controlling the shoulder, arm, and hand.
When a newborn shows weakness or limited movement in one arm after delivery, it can be frightening and confusing for parents. One possible cause is a brachial plexus injury, a condition that affects the group of nerves controlling the shoulder, arm, and hand.
Among these injuries, Erb’s palsy is the most common and well-known form.
According to the Cleveland Clinic, Erb’s palsy occurs in approximately 0.9 to 2.6 out of every 1,000 live births, which equals roughly 12,000 cases each year in the United States.
While the diagnosis can be overwhelming, there is reassuring news: most infants recover function in the affected arm, especially when improvement begins early. Understanding how these injuries occur, what symptoms to watch for, and how recovery typically progresses can help parents feel more confident and prepared as they navigate their child’s care.
What Is the Brachial Plexus?
The brachial plexus is a network of nerves that extends from the spinal cord in the neck through the shoulder and into the arm. These nerves control movement and sensation in the shoulder, arm, and hand—allowing a child to lift, bend, grasp, and feel with their upper limb.
In newborns, these nerves are delicate and still developing. During birth, the brachial plexus can stretch, compress, or even tear if the baby’s head and neck are pulled to one side while the shoulder remains stuck during delivery. This can happen when the baby is large, positioned awkwardly, or when assistance is required with tools such as forceps or a vacuum extractor.
The extent of a brachial plexus injury can vary greatly. Some babies experience only mild stretching of the nerves (a condition called neurapraxia), which often heals on its own within weeks. Others may have more severe injuries involving nerve rupture or avulsion (when the nerve root is pulled away from the spinal cord). These cases can result in longer-term weakness or paralysis of the affected arm and may require specialized treatment to promote recovery.
What Is Erb’s Palsy?
Erb’s palsy is the most common form of brachial plexus injury in newborns. It occurs when the upper portion of the brachial plexus—the nerves near the neck that control the shoulder and upper arm—is stretched or injured during birth. This can result in partial or complete weakness of the affected arm.
Typical signs of Erb’s palsy include a limp or rotated arm held close to the body, limited movement at the shoulder or elbow, and a weaker grasp in the hand on that side. The baby may not react equally when startled or when both arms are lifted, revealing an asymmetry in movement known as an asymmetric Moro reflex.
Erb’s palsy accounts for about 50 to 60 percent of all brachial plexus injuries, while more severe upper or total plexus injuries are less common. Klumpke’s palsy, a rare palsy that affects the lower plexus and hand muscles, occurs in less than 1 percent of cases.
Although the initial symptoms can be alarming, many infants experience improvement within the first few weeks of life. Early monitoring helps doctors determine which injuries are likely to heal on their own and which may need additional therapies or evaluation by a specialist.
Birth Injury Due to Medical Negligence?
Contact Our Lawyer Now for Expert Support!
How Brachial Plexus Injuries Occur During Birth
Most brachial plexus injuries happen during challenging vaginal deliveries when the baby’s shoulder becomes lodged behind the mother’s pelvic bone after the head has been delivered. This complication, known as shoulder dystocia, can place pressure on the baby’s neck and shoulder as the medical team works to safely complete the delivery.
When traction or pulling occurs—either from natural forces of labor or from assisted delivery tools such as forceps or vacuum extractors—the stretching of the baby’s neck away from the shoulder can injure the nerves of the brachial plexus. Even gentle traction can be enough to cause a temporary stretch in these sensitive nerve fibers.
Certain factors make these injuries more likely, including:
- Large birth weight or maternal diabetes (which can increase baby size)
- Prolonged or difficult labor
- Breech position, where the baby is delivered feet or buttocks first
- Instrument-assisted deliveries, which may place additional pressure on the baby’s head and shoulders
While these situations can happen unexpectedly and are often unavoidable, they may result in varying degrees of nerve injury—from mild stretching that heals within weeks to more significant damage that takes months or longer to recover. Understanding the mechanics of these injuries can help parents recognize why early evaluation and follow-up care are so important.
Early Signs Parents Might Notice
In the first days after birth, it can be difficult to know what typical newborn behavior is and what might signal a nerve injury. For infants with a brachial plexus injury or Erb’s palsy, parents and healthcare providers may observe specific signs that stand out as the baby begins to move and stretch. Some early indications may include:
- Limited movement in one arm: The baby may not lift or bend one arm as easily as the other.
- Arm held close to the body: The affected arm may rest straight and rotated inward at the shoulder.
- Weak or absent grasp: The baby’s grip in the affected hand may feel weaker.
- Asymmetric startle reflex: When startled, most babies extend both arms outward; a baby with Erb’s palsy may only move one arm.
- Differences in muscle tone: The affected arm may appear softer or less responsive.
In many mild cases, these symptoms gradually improve over the first few weeks as swelling around the injured nerves subsides. However, if little or no movement returns after the first two to three weeks, doctors typically recommend further evaluation. Tracking these signs early helps guide next steps, including therapy or imaging studies, and ensures that any lingering weakness is addressed as soon as possible.
How Doctors Diagnose Brachial Plexus Injuries
When a newborn shows weakness or reduced movement in one arm, the first step is a careful physical examination. Doctors and neonatal specialists look for characteristic signs—such as decreased shoulder or elbow movement, a weaker grasp, or differences in reflexes between the two arms. Gentle observation of how the baby moves during routine care often provides the earliest clues.
If the symptoms persist beyond the first few days, additional tests may help determine the type and extent of the injury. These can include:
- Ultrasound or MRI scans, which allow doctors to see the nerves, surrounding muscles, and soft tissues in detail.
- Nerve conduction studies and electromyography (EMG), which measure how well the nerves send signals to the muscles. These tests are usually done a few weeks or months after birth, once the nerves have had time to heal or show lasting changes.
- Range-of-motion assessments by pediatric neurologists or physical therapists, to document progress and guide treatment plans.
Diagnosis is not always immediate; some mild injuries improve so quickly that no further testing is needed, while others require months of follow-up to confirm the degree of recovery. By combining clinical observation with imaging and functional testing, doctors can tailor the right approach for each baby and determine whether therapy, monitoring, or surgical evaluation may be necessary.
Need Legal Support?
Talk to a Birth Injury Attorney for Free!
Treatment and Recovery
The outlook for infants with a brachial plexus injury or Erb’s palsy is often encouraging. Treatment depends on the severity of the nerve injury and how quickly function returns to the affected arm.
For many babies, the injury is mild, and these cases may heal on their own within the first few months. Gentle range-of-motion exercises, usually taught by a pediatric physical or occupational therapist, help prevent stiffness and encourage healthy nerve recovery. Parents are often shown how to perform these movements during daily care routines.
If improvement is limited after several weeks, or if certain muscles remain weak, doctors may recommend further evaluation by a specialist in pediatric nerve injuries. Imaging and nerve studies can show whether there is a rupture or tear that requires surgical repair.
According to clinical research, about 80–96 percent of infants experience complete recovery, especially when signs of improvement appear within the first two weeks of life. For those who need surgery, approximately two-thirds show meaningful improvement after surgical exploration and nerve reconstruction.
While recovery can take months or even years, most children ultimately regain good strength and function in the arm. A small percentage may have lasting weakness, differences in arm growth, or limited range of motion. Early therapy, consistent follow-up, and support from experienced medical professionals give children the best chance for a strong recovery and full participation in daily activities.
What Parents Can Do for Injured Children
Learning that your baby has a brachial plexus injury can be overwhelming, but there are many ways parents can support recovery at home and work alongside their child’s care team.
- Stay engaged with follow-up appointments. Regular check-ins with your pediatrician or specialists allow doctors to monitor progress, update therapy goals, and identify any lingering weakness early. Bring a list of questions to each visit and keep a folder of all test results and therapy notes for easy reference.
- Practice gentle exercises at home. Therapists often teach simple range-of-motion activities that parents can do daily to keep joints flexible and prevent muscle stiffness. Turning these exercises into playful, soothing moments—like singing or gentle massage—can make them part of your baby’s routine.
- Track small milestones. Noting when your baby begins lifting, grasping, or reaching again can help physicians evaluate nerve recovery. Many families find it encouraging to record progress in a notebook or app.
- Seek early intervention services if recommended. Programs available through local hospitals or local or state resources can provide occupational or physical therapy, adaptive support, and developmental monitoring during the early months.
- Most importantly, give yourself and your baby time. Nerves heal slowly, and gradual improvement is normal. Staying patient, observant, and connected with your medical team can make a tremendous difference in your child’s outcome and confidence. However, if you need to take legal action for your baby’s harm, keep in mind that there are legal deadlines for doing so. Stay in touch with a medical malpractice lawyer who can monitor all the deadlines for you.
Understanding what’s happening inside your child’s body—and how recovery typically unfolds—can help you feel confident and proactive as a parent. Stay connected with your medical team, celebrate every sign of progress, and remember that early support leads to the best long-term outcomes.