Table of Contents
Table of Contents
What is a Birth Injury?
A birth injury is any form of physical harm or medical complication that results in an injury to a baby shortly before, during, or immediately after delivery. These injuries can range from minor bruising or temporary nerve damage to serious conditions that affect movement, breathing, or brain function. While some birth injuries heal completely with time and care, others can lead to lifelong challenges that affect a child’s development and quality of life.
In some cases, a baby may suffer oxygen deprivation during prolonged or difficult labor. In others, excessive pressure from delivery tools such as forceps or vacuum extractors can cause nerve damage or skull fractures. Even an injury that seems minor at first—like a small bump or weakness in a limb—may later reveal a deeper problem once developmental milestones are delayed.
Are Injuries at Birth Avoidable?
It’s important to understand that not every complication during childbirth is preventable. Labor and delivery are complex processes that can involve unexpected changes in the baby’s position, heart rate, or size. However, modern obstetrics provides tools and monitoring systems that help medical teams identify and respond to risks quickly. When a healthcare provider recognizes signs of distress and takes appropriate, timely action, many serious outcomes can be avoided.
But when those responses are delayed or mismanaged, the baby may be left with preventable injuries that alter the course of their life. Not all complications present at birth share the same cause. Some result from trauma during delivery, while others stem from genetic or developmental factors. Knowing the difference between a birth injury and a birth defect can bring clarity—and peace of mind—during an uncertain time.
What is the Difference Between a Birth Injury and a Birth Defect?
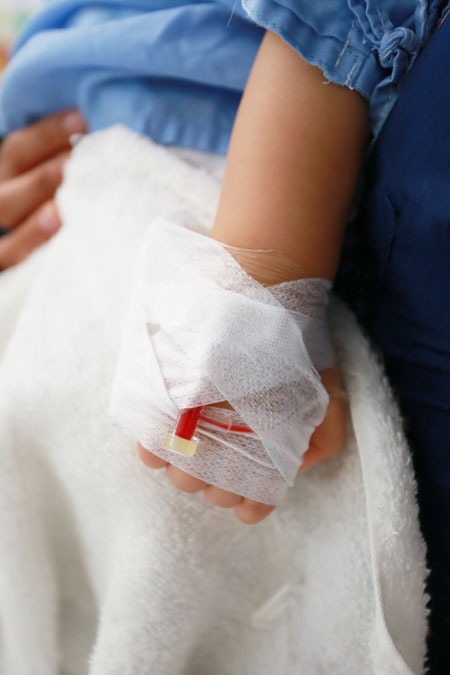
- Congenital heart defects
- Cleft palate
- Spina bifida
In most cases, birth defects are not caused by anything that happens during labor or by the actions of medical providers. They may be detected through prenatal testing, such as ultrasounds or genetic screening, though some are not apparent until after birth.
A birth injury, on the other hand, occurs during the process of labor or delivery. Sometimes those events are unavoidable, even when skilled professionals take all appropriate precautions. But other times, a birth injury may occur when:
- Warning signs are missed
- Conditions are not diagnosed or treated
- Labor is allowed to progress too long
- Medical tools or maneuvers are used with too much force or at the wrong time.
These injuries are typically the result of physical trauma, lack of oxygen, and complications that develop during the birth itself. It is important to note that there are some conditions during pregnancy that can increase the likelihood of birth injuries if a medical professional does not address these issues.
Parents don’t need to make this distinction on their own. Pediatricians, neurologists, and developmental specialists can help determine whether a child’s condition appears to be the result of a prenatal defect or a delivery-related injury. The right testing, imaging, and developmental evaluations can clarify when the harm occurred and what steps might support recovery or long-term care.
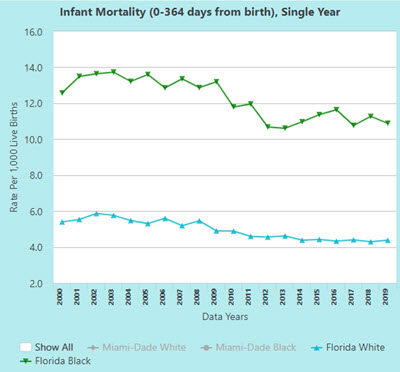
Birth Injuries by the Numbers
Behind every birth injury is a deeply personal story—but looking at the broader data helps families understand just how significant these issues are nationwide. Birth injuries are uncommon compared to the total number of deliveries each year, yet they remain a leading cause of long-term developmental and neurological challenges in infants.
How Often Birth Injuries Occur
Large-scale studies estimate that neonatal birth trauma affects roughly 25–31 infants per 1,000 hospital births in the U.S., with rates rising slightly in recent years. The majority of these involve scalp or soft-tissue injuries, which make up about 80% of all reported cases. While most of these injuries can be resolved without lasting harm, they can sometimes signal deeper issues such as oxygen deprivation or intracranial bleeding.Major birth trauma—including fractures, nerve injuries, and internal hemorrhages—occurs in approximately 4–5 out of every 1,000 births, representing a smaller but more serious subset. These cases are often associated with higher rates of hypoxic-ischemic encephalopathy (HIE), seizures, and longer hospital stays.
Instrument Use and Delivery Complications
Tools such as forceps and vacuum extractors are sometimes used to assist with difficult deliveries, but they also increase the risk of certain injuries.Research shows that subgaleal hemorrhage, a rare but potentially life-threatening bleeding between the scalp and skull, occurs in 0.6 per 1,000 births overall, but the rate jumps to 4.6 per 1,000 in vacuum-assisted deliveries. Other studies report rates as high as 7 per 1,000 following vacuum use, underscoring the importance of careful selection and monitoring when these tools are applied.
Fractured clavicles—often the result of shoulder dystocia or challenging vaginal deliveries—are among the most common major injuries, affecting about 0.5–1% of all vaginal births, or up to 10 per 1,000 deliveries. In higher-risk situations, the rate can be even greater.
Neurological and Oxygen-Related Injuries
Among the most serious complications are those linked to oxygen loss during labor. Hypoxic-ischemic encephalopathy (HIE) occurs in roughly 1–2 per 1,000 births in high-income countries, though global estimates reach up to 12 per 1,000. HIE contributes to about one million neonatal deaths worldwide each year and is a leading cause of long-term neurological disability.The Centers for Disease Control and Prevention estimates that cerebral palsy affects between 1.5 and 4 per 1,000 live births. In the U.S., that translates to roughly one in every 345 children—nearly one million Americans are living with CP today.
Maternal and Infant Risk Factors
Several well-documented risk factors increase the likelihood of birth complications. In recent CDC data, about 8.6% of newborns were born with low birth weight, and 10% were premature, both of which heighten vulnerability to oxygen-related injuries. Prolonged labor—affecting roughly 8% of deliveries—can also increase the chance of distress or mechanical trauma during birth.Other neonatal conditions, while often treatable, highlight how fragile the first days of life can be. Jaundice affects around 60% of term infants and up to 80% of preterm babies, though severe complications such as kernicterus are now rare, occurring in about 1 in 44,000 births in high-income countries.
While statistics provide valuable insight, they don’t capture the full impact of a birth injury on a family’s life. Behind each data point is a child whose development, medical needs, and daily care may be shaped by the events of a single day.
When an Injury May be a Result of Substandard Care
Childbirth is unpredictable, and not every complication points to medical negligence. Even with careful monitoring, some emergencies develop suddenly and require rapid decisions under pressure. Still, there are situations where an injury could have been avoided had the appropriate medical standards been followed. Understanding what constitutes substandard care can help families ask informed questions and seek clarity about what happened during labor and delivery.
In healthcare, “standard of care” refers to the level of attention, skill, and judgment that a reasonably competent professional would provide under similar circumstances. When providers follow accepted medical guidelines, they help ensure a safe outcome for both mother and baby. Substandard care occurs when those expectations are not met, and as a result, the patient experiences harm. Examples of substandard care during childbirth can include:
- Failure to recognize fetal distress. Continuous heart rate monitoring is a key part of labor management. When warning signs, such as prolonged decelerations, are ignored or misinterpreted, oxygen deprivation can result.
- Delayed response to delivery complications. Certain emergencies, including shoulder dystocia or cord compression, require immediate action to prevent injury.
- Improper use of delivery instruments. Forceps or vacuum extractors can be valuable tools, but when used with too much force or at the wrong angle, they may cause nerve or skull injuries.
- Failure to order or perform a timely cesarean section. In cases where vaginal delivery poses risks to the baby’s health, a delay in performing a C-section can have serious consequences.
- Inadequate maternal monitoring. Maternal conditions such as preeclampsia, infection, or gestational diabetes can heighten the risk of infant injury if not carefully managed.
Some injuries happen despite excellent care and immediate intervention. However, when communication breaks down, when crucial signs go unaddressed, or when delivery decisions fall outside established medical practice, the standard of care may have been compromised.
Early Signs of a Birth Injury in Your Newborn
Every parent hopes for a smooth delivery and a healthy baby. But sometimes, a newborn’s first hours or days bring unexpected challenges. Some signs of a possible birth injury appear right away, while others unfold gradually as your child grows. Recognizing early indicators doesn’t mean assuming the worst; it means understanding your baby’s needs and ensuring they receive the right care as soon as possible.
At Birth
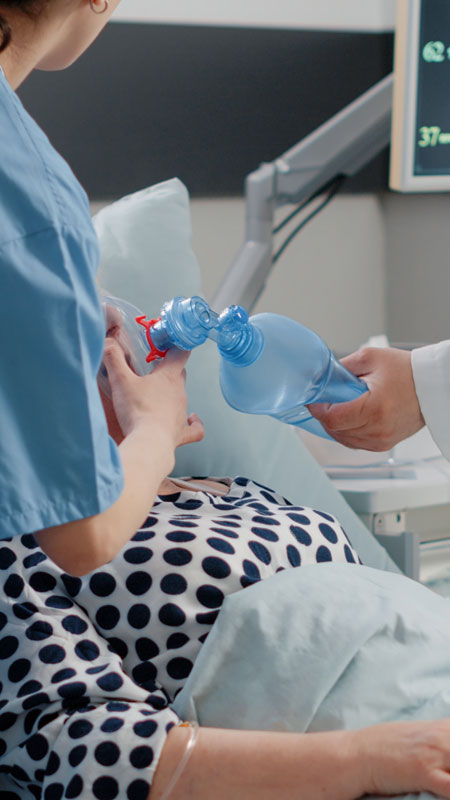
- If your baby has trouble crying, seems unusually still or limp, or has difficulty breathing, the medical team may perform additional tests or interventions.
- Bruising, swelling, or marks on the head or shoulders can result from difficult deliveries or the use of forceps or vacuum extractors.
- Limited movement in one arm or leg, especially if paired with crying when that limb is touched, may indicate a nerve or muscle injury such as brachial plexus damage.
- Other times, a newborn may appear healthy but exhibit subtle warning signs: poor muscle tone, pale or bluish skin color, or weak reflexes.
These symptoms can sometimes point to oxygen deprivation during delivery, which deserves close monitoring and follow-up testing.
First 72 Hours
The first three days after birth are often a critical period. During this time, certain symptoms may emerge as your baby’s body adjusts.
- Difficulty feeding, persistent lethargy, irregular breathing, or unusual jitteriness can suggest that something deeper is affecting the nervous system.
- Low Apgar scores—evaluations of breathing, heart rate, reflexes, muscle tone, and color—may also prompt doctors to observe your baby more closely.
- Seizures, extreme irritability, or stiffness in the arms or legs can indicate potential brain injury or bleeding.
In some cases, these symptoms may appear hours after a seemingly routine delivery. Because early treatment can significantly improve outcomes, it’s essential that newborns showing any of these signs are evaluated by specialists right away.
First Six Months
Not all birth injuries are apparent in the hospital. As your baby grows, developmental milestones provide important clues about how well their brain and body are communicating. By six months, most infants have begun rolling over, reaching for toys, holding up their heads, and responding to familiar voices and faces.
If your baby struggles to meet these milestones, has trouble focusing their eyes, consistently favors one side of the body, or seems unusually stiff or floppy, these may be signs of an underlying neurological or muscular issue. Parents often notice small but telling differences—a clenched fist that doesn’t relax, difficulty feeding, or a lack of cooing or social engagement.
While some delays resolve naturally, others benefit from early intervention services such as physical or occupational therapy. Tracking your child’s progress and sharing any concerns with pediatric specialists can make an enormous difference in diagnosis and treatment planning.
Tests That Help Doctors Understand Your Baby’s Health
When newborns show unusual symptoms or delayed responses, doctors rely on a series of clinical tests to assess their health and neurological function. These evaluations help distinguish between temporary adjustment issues and more serious injuries that may require treatment or ongoing care.
Apgar Scores

- Appearance (skin color)
- Pulse (heart rate)
- Grimace (reflex response)
- Activity (muscle tone)
- Respiration (breathing effort)
Each category receives a score from 0 to 2, with a total score ranging from 0 to 10. A baby who scores between 7 and 10 is typically considered to be adapting well. Scores below 7 may indicate difficulty transitioning and prompt closer monitoring or medical intervention.
A low Apgar score doesn’t always mean a baby has a lasting injury—it may simply reflect a brief period of distress during birth. However, persistently low scores, especially at five months or later, can signal oxygen deprivation or other complications that may warrant further neurological evaluation.
MRI, Ultrasound, EEG, and Hearing/Vision Screenings
If a newborn shows unusual reflexes, weakness, or irregular breathing patterns, physicians may order imaging or neurological tests to gather more information.
- Magnetic Resonance Imaging (MRI) is often the most informative tool for assessing possible brain injury. It uses magnetic fields to produce detailed images of brain tissue, revealing patterns consistent with oxygen deprivation, bleeding, or stroke. MRIs are particularly valuable within the first two weeks of life, when certain types of damage can still evolve or resolve.
- Cranial ultrasound can identify swelling, bleeding, or fluid accumulation inside the brain. It’s often used in neonatal intensive care units (NICU) because it doesn’t require sedation.
- Electroencephalography (EEG) records electrical activity in the brain and helps detect abnormal patterns that might indicate seizures or underlying neurological dysfunction.
In addition to these neurological tests, newborns routinely undergo hearing and vision screenings. Failure to respond to sound or track movement may point to sensory impairments or central nervous system involvement. When results are abnormal, doctors typically repeat the test or refer the family to pediatric specialists for further assessment.
When Test Results Warrant Further Action
Each of these evaluations offers a piece of a larger picture. When test results show patterns such as persistent low Apgar scores, abnormal MRI findings, or seizure activity on EEG, doctors may recommend follow-up imaging or developmental monitoring.
Early detection of neurological or physical injury allows families to begin interventions sooner. For example, babies with early evidence of muscle stiffness or weakness may start physical therapy within months of birth. Those with signs of hearing loss can receive early auditory support that helps prevent language delays.
Parents should feel encouraged to ask for copies of test results, imaging reports, and discharge summaries. Keeping records organized helps ensure that any specialist who later evaluates the child has access to the full medical history. These documents can also assist developmental therapists and pediatricians in tracking progress and making evidence-based care recommendations.

Read our free guide about the most common things you should know about birth injuries.
Understanding What Can Go Wrong During Birth — and Why
Even with modern monitoring and skilled professionals, childbirth can be unpredictable. Labor sometimes progresses too slowly, a baby may show distress, or delivery may require intervention. These moments call for careful observation and prompt decisions. Many injuries occur not from a single mistake but from small, compounding delays when timing is critical.
Fetal Distress and Delayed Response
During labor, a baby’s heart rate provides real-time insight into oxygen and blood flow. Fetal distress occurs when the pattern shows the baby isn’t tolerating contractions well, often due to umbilical cord compression, prolonged labor, or overly strong contractions.
Medical teams monitor these patterns and can take steps to stabilize the baby, such as repositioning the mother, adjusting medications, or moving to an emergency delivery. If the distress continues without timely action, oxygen deprivation can develop, setting the stage for possible neurological complications later.
Shoulder Dystocia
Shoulder dystocia happens when the baby’s shoulders become lodged behind the mother’s pelvic bone after the head is delivered. It’s an unpredictable but serious emergency that requires calm, skilled maneuvers to release the shoulder.
Because this can happen suddenly, every delivery team should know how to respond within seconds. The danger arises when improper traction or excessive pulling is used, increasing the risk of nerve or skeletal injury. Good preparation and communication among providers are key to managing this event safely.
Instrument-Assisted Delivery
When labor slows or the baby shows distress, doctors may use forceps or a vacuum extractor to assist. These tools can be lifesaving when used correctly, but risky when used too forcefully, too often, or too late in labor.
Pressure from these instruments can cause scalp or skull trauma, especially if multiple attempts are made. Following clinical guidelines—such as limiting attempts and switching to cesarean when needed—reduces the risk of harm.
Maternal Complications That Increase Risk
Some complications originate not with the baby but with the mother’s health during labor. Preeclampsia, gestational diabetes, infection, or placental abruption can disrupt oxygen and nutrient flow to the fetus.
When maternal health conditions are detected and managed promptly, outcomes are usually good. But when warning signs go unnoticed or aren’t addressed quickly, both mother and child can face serious consequences. Monitoring maternal vitals as closely as the baby’s remains one of the best safeguards in obstetric care.
A population study of more than six million births found that mothers of children later diagnosed with cerebral palsy were significantly more likely to have had infections during pregnancy or delivery (13.7%) compared to mothers of children without CP (5.5%). Infections showed higher CP risk, reinforcing the importance of early screening and treatment during pregnancy. When labor complications are recognized and managed early, most birth injuries can be avoided. When they’re not, the resulting harm can take many forms.
Common Conditions Linked to Delivery Errors
When complications during birth interrupt a baby’s oxygen supply or cause physical trauma, the effects may emerge immediately or over time. Some infants recover fully with supportive care, while others develop conditions requiring long-term treatment. Understanding these medical outcomes helps families anticipate challenges and pursue early interventions.
Cerebral Palsy
Cerebral palsy (CP) can result from oxygen deprivation or brain bleeding during labor. It affects muscle tone, posture, and coordination, often leading to delayed movement or stiffness. While CP is not progressive, symptoms become more noticeable as children grow.
Children with CP can face a wide range of related challenges. The Cerebral Palsy Alliance Research Foundation reports that about half of children with CP have an intellectual disability, around one-third cannot walk independently, and one in four experience epilepsy or significant speech difficulties. Many also live with pain, sleep disorders, or other health complications that require ongoing management.
Despite these hurdles, early therapy, adaptive technology, and coordinated medical support can dramatically improve mobility, communication, and independence—helping children achieve meaningful progress and lead fulfilling lives.
Erb’s Palsy and Other Brachial Plexus Injuries
In difficult deliveries, especially those involving shoulder dystocia, the nerves connecting the neck and shoulder can stretch or tear. This injury, called Erb’s palsy, may cause weakness or paralysis in one arm. Physical therapy can help many children regain strength, though severe cases may require surgery to repair nerve damage.
Studies show that about 80–96% of infants with brachial plexus injuries experience full or near-full recovery within the first year of life, especially with early therapy and careful follow-up. However, any failures to identify the condition or treat it could prevent a child from full levels of recovery.
Hypoxic-Ischemic Encephalopathy (HIE)
HIE occurs when the brain doesn’t receive enough oxygen or blood flow during delivery. Depending on how long the deprivation lasts, outcomes can range from mild developmental delays to severe neurological impairment. Treatments like therapeutic hypothermia, started within hours of birth, can sometimes limit damage. Read our case study “Hypoxic-Ischemic Encephalopathy (HIE) in Newborns: National Incidence and Trends” to learn more.
Intracranial Hemorrhages
Bleeding inside the skull (intracranial hemorrhage) during or shortly after can result from mechanical stress, pressure fluctuations, or weakened blood vessels. Some infants with mild hemorrhage recover with little or no long-term impairment.
However, in more severe cases, complications may develop, such as hydrocephalus (excess cerebrospinal fluid accumulation) or seizure disorders. Lifelong neurologic follow-up, appropriate medications, and rehabilitative therapy are often part of the child’s care plan.
Complications from Maternal Health Conditions
A mother’s health directly affects the baby’s stability during delivery. When preeclampsia, infection, or placental issues are not controlled, infants can suffer oxygen deprivation or circulatory problems that contribute to brain or organ injury. Early recognition of maternal symptoms and continuous monitoring of fetal health are essential in preventing these outcomes.
Each of these conditions presents unique challenges. Some improve significantly with therapy and medical support, while others require lifelong management. Recognizing early signs and connecting with specialists as soon as possible can greatly influence a child’s long-term development.
What Parents Can do after a Complicated Delivery
Learning that your newborn may have experienced a birth injury can feel overwhelming. Between medical jargon, uncertain outcomes, and a blur of hospital visits, it’s easy to feel lost. Taking small, steady steps—asking questions, gathering information, and seeking guidance—can help you regain a sense of control. Every action you take now can make a meaningful difference in your child’s care and long-term development.
Questions to Ask at Upcoming Medical Visits
Your pediatrician is often the first ongoing point of contact after discharge, and open communication is essential. Don’t hesitate to ask direct questions, even if they seem basic or repetitive. Clear answers can reveal whether your child’s symptoms are typical or warrant further evaluation.
Helpful questions might include:
- How is my baby’s muscle tone, reflexes, or coordination compared to other infants their age?
- Do you notice any developmental delays or asymmetries?
- Should we schedule additional imaging or specialist consultations?
- Are there therapies or early intervention services you recommend starting now?
Bringing a written list of questions to each appointment helps you stay organized and ensures nothing gets overlooked in the moment. If something feels unclear, ask the doctor to explain in plain language or show examples of what’s normal versus concerning. Remember, your role as a parent includes being an advocate for your child’s health.
Requesting and Organizing Your Records
Medical documentation is one of your strongest tools for understanding what happened during labor and delivery. Hospitals and clinics keep detailed records, including fetal monitoring strips, Apgar scores, imaging reports, and neonatal intensive care notes. These materials can provide valuable insight into how your baby responded during and after birth.
Parents have the right to request copies of these records. When you do, ask for:
- Labor and delivery notes
- Fetal heart monitoring data
- Neonatal charts and discharge summaries
- Imaging results (MRI, ultrasound, EEG)
- Reports from any specialist consultations
Create a binder or secure digital folder with sections for prenatal records, delivery documentation, postnatal care, and therapy progress notes. Keep a simple log of appointments and observations, making sure to include dates, concerns raised, and what the doctor advised. Having this information accessible makes it easier to track your baby’s development and communicate effectively with future care providers.
Getting Second Opinions and Early Therapies
When a diagnosis is uncertain or you feel uneasy about your baby’s progress, a second opinion can provide reassurance or reveal new options. Pediatric neurologists, developmental specialists, and rehabilitation physicians each bring different perspectives that can help clarify what your child needs most.
Early intervention is often one of the most powerful tools for improving outcomes. Programs available through Florida’s Early Steps system or private pediatric therapy centers can evaluate your child’s motor, speech, and sensory development. Interventions can begin as early as a few months old, promoting stronger coordination, communication, and confidence.
Trust your instincts—no one knows your child better than you do. If something doesn’t feel right, continue seeking answers. Acting early doesn’t just support your child’s physical development; it can also bring comfort in knowing you’re taking every possible step toward their well-being.
Your Family Deserves Justice
Contact Our Experienced Legal Team Today!
Understanding Your Options after a Complicated Birth
When a baby experiences a preventable injury at birth, families often face not just medical and emotional challenges, but complex questions about what went wrong. In Florida, healthcare providers are expected to follow professional standards designed to protect both mother and child. When those standards aren’t met, and harm occurs as a result, families have the right to seek answers and accountability.
Understanding Patient Rights
Every parent has the right to know how their delivery was managed, what complications occurred, and how medical decisions were made in real time. Hospitals and physicians are required to maintain accurate records of the birth process, including fetal monitoring, interventions, and the sequence of events leading to delivery.
Parents can request these records and review them with trusted medical professionals to better understand what took place. Sometimes, the information shows that an injury was unavoidable. Other times, it may reveal that critical warning signs were missed or responses were delayed. Either way, reviewing the full medical picture is an important first step toward closure and informed decision-making about next steps.
The Standard of Care in Childbirth
The standard of care is a benchmark used to evaluate whether healthcare providers acted as a reasonably careful professional would have under similar circumstances. In obstetrics, this includes continuous monitoring of fetal well-being, timely responses to distress, proper management of labor progression, and safe use of medications or delivery tools.
If a provider deviates from these standards, it can result in lasting harm. Establishing whether that deviation occurred usually involves reviewing medical records and consulting with experts who understand both the medical and ethical responsibilities of obstetric care.
Presuit and Timing Requirements
In Florida, medical negligence cases follow a detailed process designed to verify that claims are supported by evidence before they ever reach a courtroom. This process is known as the presuit investigation and notice period.
Before any formal filing can occur, families (through their representatives) must:
Conduct an independent investigation to determine whether reasonable grounds exist to believe that malpractice occurred and caused injury.
Obtain a verified medical opinion from a qualified expert in the same specialty confirming that the standard of care may have been breached.
Serve a notice of intent to initiate litigation on each potentially responsible healthcare provider, which begins a 90-day presuit period.
During that 90-day window, each provider or insurer has the opportunity to investigate the claim internally, exchange records, and decide whether to settle, deny, or request arbitration. This step is meant to encourage early resolution and reduce unnecessary litigation—but it can also add months to the overall timeline.
Florida law also imposes strict time limits, known as statutes of limitations, for bringing medical negligence actions. Generally, the clock begins when the injury is discovered—or reasonably should have been discovered—but several exceptions can apply, especially in cases involving children or delayed diagnosis. Because these rules are complex, families may lose their right to pursue accountability if deadlines expire.
For that reason, once parents begin to suspect that something went wrong during pregnancy, labor, or delivery, it’s crucial to contact an attorney right away so they can gather medical records, obtain expert review, and conduct the necessary investigation as early as possible. Acting within these rules preserves the family’s ability to seek answers later, even if they are still focused on their child’s immediate care and recovery.
Seeking Support
Exploring whether a medical error contributed to a child’s condition doesn’t have to happen right away, and families should never feel rushed. The most important step is to focus on the child’s care, early therapies, and emotional well-being. When the time feels right, parents can begin gathering records and exploring their options with professionals who specialize in understanding complex birth outcomes.
Having knowledgeable support during this process can make it easier to interpret medical findings and understand potential next steps. Whether that leads to a clearer understanding of what happened, or formal accountability measures, the goal remains the same: ensuring that every child receives the care, resources, and justice they deserve.
FAQ – Frequently Asked Questions
Can Children Outgrow the Effects of a Birth Injury?
Some children recover fully from mild birth injuries, while others may face long-term effects that require ongoing care. The outcome depends on the type and severity of the injury, how quickly it’s identified, and how early therapies begin. Nerve injuries and minor muscle weakness often improve within weeks or months.
More serious injuries, such as those affecting the brain or central nervous system, may not resolve completely but can be managed with physical, occupational, and speech therapy. Every child’s recovery path is unique, and early intervention offers the best chance for improvement.
How Can I Tell the Difference Between a Normal Newborn Delay and Signs of a Birth Injury?
Every baby develops at their own pace, so small differences don’t always signal a problem. However, consistent patterns—like stiffness or floppiness, poor feeding, weak reflexes, or favoring one side—may indicate a neurological or muscular issue. Pediatricians use milestone tracking, reflex testing, and developmental screenings to determine if a delay is within the normal range or needs further evaluation.
If you’re ever unsure, bring your concerns to your child’s doctor and keep notes on what you observe at home. Trust your instincts—parents often notice subtle changes before anyone else.
Can Birth Injuries Appear Months After Delivery?
Yes. Some birth-related injuries, especially those affecting the brain or nervous system, don’t show up right away. The first signs may appear as your child misses key developmental milestones, such as holding up their head, rolling over, or grasping toys.
Subtle delays in communication, coordination, or movement can also emerge over time. These gradual signs often lead to a diagnosis months later, once the pattern becomes clear. Regular pediatric checkups, milestone tracking, and open communication with your doctor are essential to catching early concerns before they become more serious.
What Should I Do If I Suspect My Child’s Injury Happened During Birth?
Start by organizing your child’s medical records, including delivery notes, hospital discharge summaries, and any imaging or lab results. Document your child’s symptoms, developmental milestones, and therapy progress. Then, share this information with your pediatrician or a specialist for a detailed review.
Even if the connection to birth isn’t immediately clear, having comprehensive documentation helps professionals assess what might have happened and guide the next steps. Most importantly, continue your child’s medical care; early evaluation and therapy are the most valuable tools for supporting recovery.
What Resources Exist for Parents of Children with Birth-Related Disabilities?
Families don’t have to navigate this journey alone. Florida’s Early Steps program, United Cerebral Palsy, and the March of Dimes all provide information, therapy access, and support groups. Many hospitals also offer social work services to connect families with financial and emotional resources.
Online and local parent networks can be invaluable for sharing advice, finding community, and accessing early childhood programs. Taking advantage of these resources helps families focus less on red tape and more on supporting their child’s progress.
How Do I Talk to Doctors If I’m Worried About My Baby’s Care During Delivery?
It’s natural to have questions after a difficult birth. Start by calmly explaining your concerns and asking for a review of your baby’s delivery and hospital records. You can request copies of fetal monitoring reports or neonatal notes for your own understanding.
If you feel your questions aren’t being answered, ask to speak with a patient advocate or seek a second opinion. Most providers welcome engaged, informed parents. Clear communication helps everyone work toward the same goal: your baby’s health and well-being.
Disclaimers
Medical Disclaimer
The medical information provided on this site is for educational purposes only and is not professional medical advice. Using this site does not establish a doctor-patient relationship. We make no representations or warranties about the accuracy or completeness of the medical information provided. Always seek the advice of a licensed healthcare provider for any medical condition and verify any medical information with qualified healthcare professionals.
Legal Disclaimer
The content on this website is for informational purposes only and should not be construed as legal advice. Every case is unique, and you should consult a qualified attorney about your specific legal case. Past results do not guarantee or predict future outcomes. The facts and circumstances of your case may differ from the matters in which these results were obtained. Every case is different, and each client’s case must be evaluated and handled on its own merits. Prospective clients may not obtain the same or similar results. Past result amounts represent gross verdicts and settlements obtained on behalf of our clients, without adjustment for fees, costs, or medical liens.
Contacting us through this website or submitting information does not establish an attorney-client relationship. Do not share any confidential information with our firm or any other until an attorney-client relationship has been formally established in writing.